
Access to Victorian hospital emergency departments has become steadily worse since 2013, an Auditor-General's report has found.
Subscribe now for unlimited access.
or signup to continue reading
The analysis revealed the state's hospitals only met one of their five key targets across the decade, and failed on the other four every single year.
One of the metrics - the number of people staying longer than 24 hours in ED - rose more than 2000 per cent over the decade to 11,363 patients.
The government target was zero.
This problem was twice as bad in regional health services, with Ballarat Base Hospital the worst offender, but wait times were also poor in Bendigo, Geelong, Warrnambool and Mildura.
The report included case studies looking at the specific challenges for Ambulance Victoria, Royal Melbourne Hospital, Werribee Mercy Hospital, and Bendigo Health.
It analysed eight measures the government had taken to fix the problems, but found no "significant improvement".
The Auditor-General made three recommendations to improve the system, including investigating what's causing the problems and publishing better public data on ED wait times.
The state government has accepted two recommendations in full and one "in principle" and said it had already started work to meet them.
A government spokesperson blamed COVID-19 for the failures.
"Health systems across the world have been heavily impacted and changed as a consequence of the one-in-100-year pandemic," the spokesperson said.
10 years of missed targets
The Victorian government published five "key performance measures" for ED access:
- Seeing patients within the clinically recommended time frame - (target 80 per cent)
- Patients staying in ED longer than 24 hours - (target 0)
- Patients being transferred from an ambulance to ED within 40 minutes - (target 90 per cent)
- Patients with length of stay in ED of less than four hours (target 81 per cent)
- Category 1 patients (those with immediately life-threatening conditions) being seen immediately - (100 per cent)
The state's hospitals met the fifth target - seeing critically ill patients immediately - consistently between 2013-14 and 2022-23.
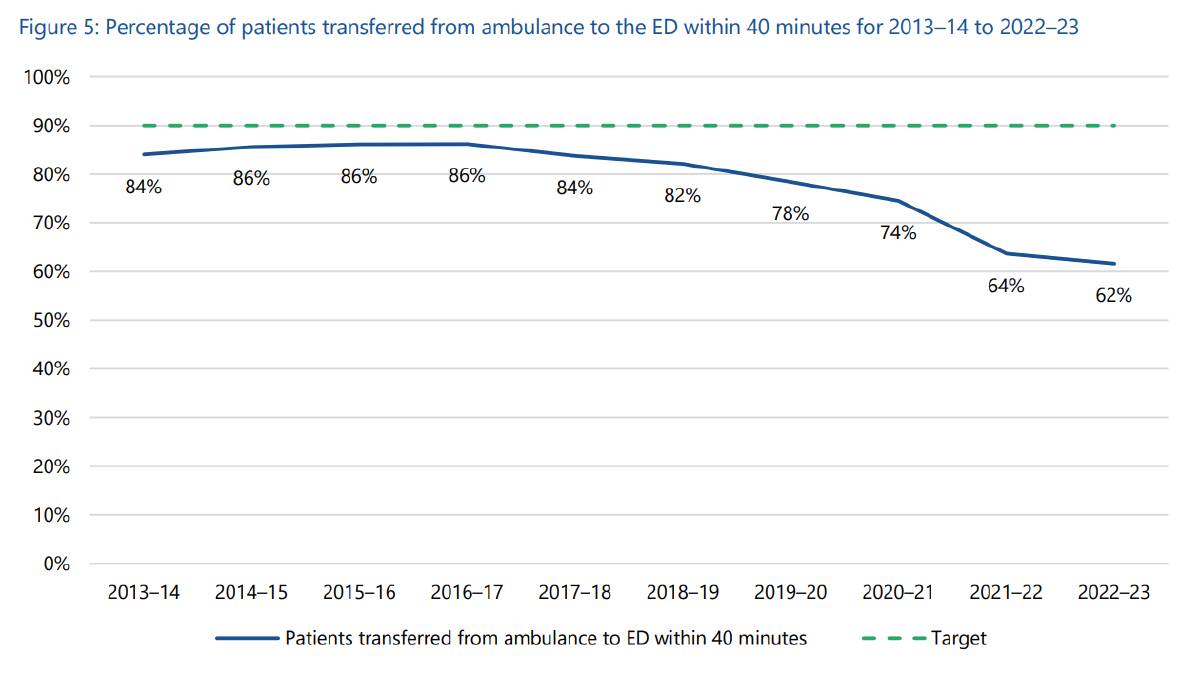
It failed every other target every year across the decade, with results also getting progressively worse over the 10 years.
Between 2014 and 2017 about 86 per cent of patients were transferred from ambulances within 40 minutes, which was close to the 90 per cent target.
By 2023 it had dropped to 62 per cent as ambulance ramping became a serious issue in Melbourne and major regional centres like Ballarat and Bendigo.
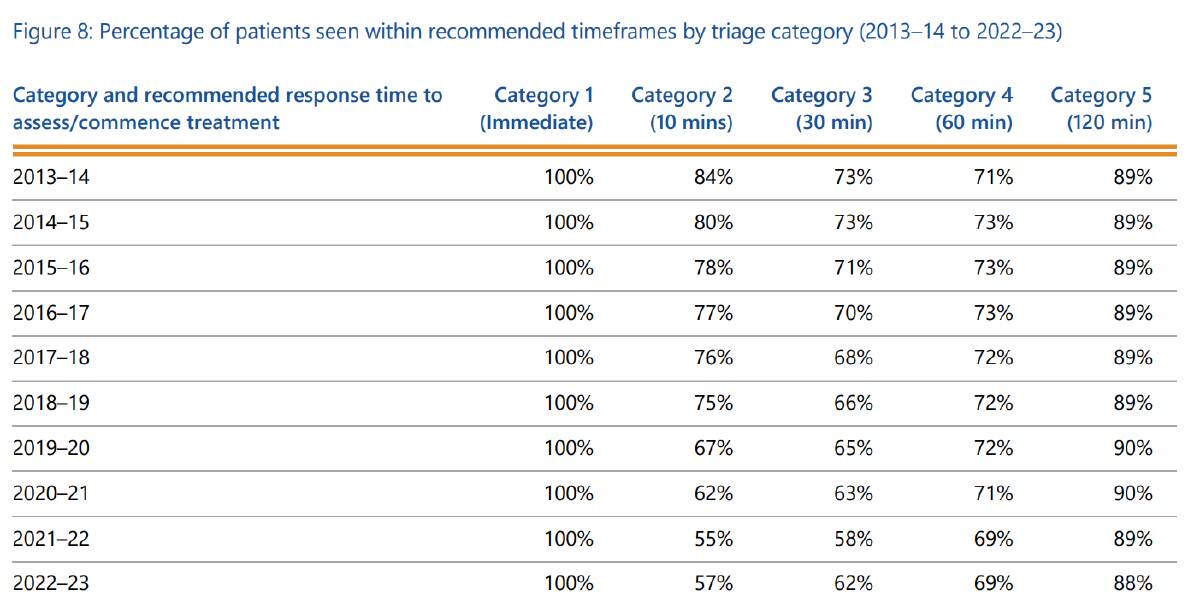
The percentage of patients seen within the recommended time frames also dropped steadily over the decade from 75 per cent in 2013 to 63 per cent in 2022.
It rebounded to 65 per cent in 2023 but the report said it was unclear whether this was a blip or a sustainable improvement.
While Category 1 patients were always seen immediately, Category 2 patients - those with "imminently life-threatening conditions", who should be treated within 10 minutes - had the worst drop off of any category, falling from 84 per cent to 57 per cent.
The percentage of patients getting treatment and leaving ED within four hours also dropped steeply from 2016, going from 71 per cent to 52 per cent in 2023. The government-mandated target is 81 per cent.
Regional worries
But it was the number of patients staying longer than 24 hours in ED that deteriorated most over the 10-year audit period.
In 2013-14 the figure was 518, and it dropped to 292 four years later in 2017-18.
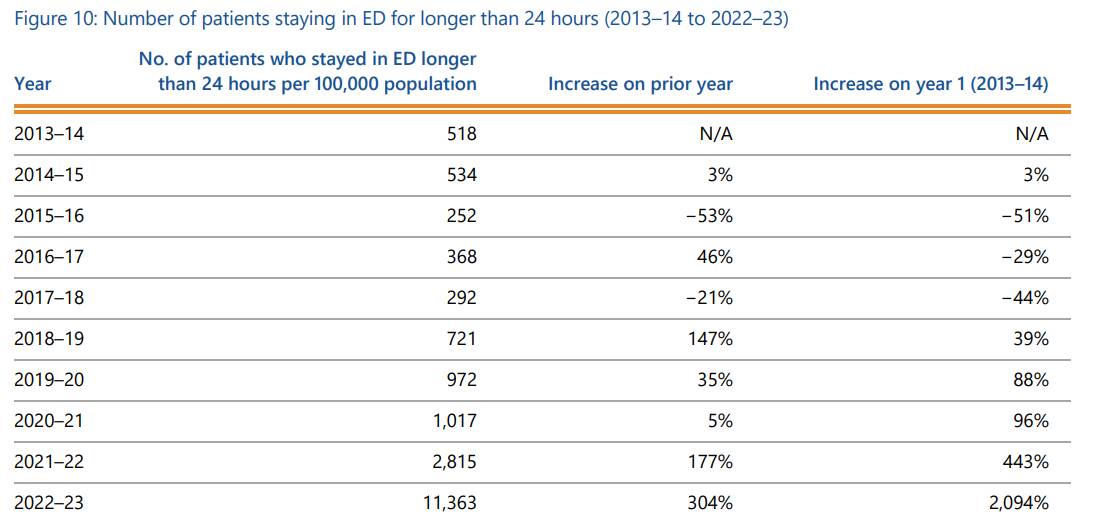
But by 2019-20 it had tripled to 972 and during COVID it blew out to 11,363, 22 times higher than it had been 10 years before.
The government-mandated target is to have zero patients stay longer than 24 hours.
The report found regional patients were twice as likely as metro patients to endure ED stays longer than 24 hours.
The state government said a handful of regional hospitals were responsible for the spike.
Recent data showed Ballarat Base Hospital was the worst in Victoria on that measure for much of 2023.
The hospital had nearly 1600 patients stay longer than 24 hours in ED from April to December 2023.
The next highest was Monash Medical Centre with less than 1000, even though Monash treated twice as many patients over that period.
The government said it was engaging with the hospitals responsible for most of the "24 hour breaches" to work out what was going wrong and fix the issues.
Ballarat's figures improved significantly in the first three months of 2024, but the Auditor-General said longer term data was necessary to demonstrate a sustainable improvement.
Ballarat also recorded the worst proportion of patients seen within the recommended time of any regional hospital in 2023. It was also the second worst in the state behind Werribee Mercy Hospital.
Werribee was highlighted in the report as an undersized hospital facing unique challenges of huge population growth, sicker patients, and drug and alcohol problems.
The report also looked closely at the factors leading to poor results at Bendigo Health.
It found population growth in Bendigo's catchment area was an ongoing challenge, along with the ageing population and poor access to GPs, especially bulk billing GPs.
Aside from those demand factors, patient flow was an increasing problem, with "bed block" due to the lack of timely discharge from hospital wards making it difficult to admit patients from ED.
Recent "code yellow" events - an internal emergency where the hospital can't cope with demand - at Bendigo Health demonstrate demand and patient flow remains a problem.
No significant improvement
The state government has launched a range of programs in the past three years to try to relieve pressure on the hospital system and EDs in particular.
The Victorian Virtual Emergency Department has helped less sick patients get timely care without putting demand on emergency waiting rooms, while Priority Primary Care Centres have partially made up for a chronic lack of GPs, especially in the regions.
The government has also put millions of dollars into pathways to home programs to help support patients to recuperate at home rather than in hospital.
The audit found while these programs had helped divert patients from EDs and hospital beds, it hadn't translated to an overall improvement in the performance data.
The report said there was no sign the systemic challenges would improve.
"Given the increasing proportion of higher-acuity presentations, demand will likely continue to put significant pressure on our state's EDs, and therefore on the broader hospital system," it said.
The government has already started work to analyse and address the factors driving its ongoing failure to meet its own performance targets.
But it opted not to fully accept the Auditor-General's recommendation to improve its public data monitoring.
The report said the government should publish long-term performance data, rather than the 15 months of data it currently provides.
The government agreed "in principle", but refused to say why it wouldn't agree in full. It has committed to publishing data going back to 2018-19, which is far less than what the NSW government provides.


